Tomorrow, Rachel and I celebrate our first wedding anniversary. With my slow writing pace, it’s taken most of that time to chronicle our honeymoon adventures in Bolivia and Peru. Part of the reason I haven’t written more of late is that we’re expecting to welcome our first child, code named Belly Buddy, who is due today.
Aside from developing a slightly high level of amniotic fluid, the pregnancy had gone very well until Week 37 when baby flipped out of head down position to breech. During the following week, baby alternated between breech and transverse. With baby growing bigger, it seemed unlike that he or she would be flipping back to the right position. Our OB, Dr. D, has a warm smile and a soft, reassuring voice. But her words this time were difficult to hear: she proposed that we schedule a c-section.
Having done a lot of reading on baby stuff, Rachel countered by suggesting an external cephalic version to manually re-position the baby. Dr. D said most providers wouldn’t even attempt such a procedure after 37 weeks, but agreed to try. But, she said, we would need to have a c-section scheduled afterward if the version failed. The procedure was scheduled for the beginning of Week 39.

MONDAY
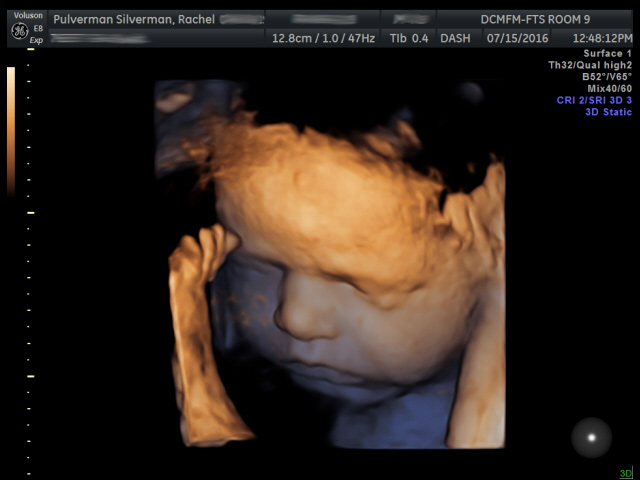
Long before dawn on the appointed day, we drove to Christiana Care Hospital. We arrived at 4:50am Rachel Standard Time (in other words, late). About half an hour later, the string of indignities—that all pregnant women eventually face—began in earnest when Rachel had to change into a baggy hospital gown. She was then hooked up to a baby monitor. A resident performed an ultrasound which confirmed that baby’s head was in the right upper abdominal quadrant. Baby was hiccuping, as was audible on the monitor. Prior to the pregnancy, I had no idea babies did this!
A nurse started an IV and a student nurse anesthetist arrived to give Rachel an epidural. This was somewhat ironic, because she’d been planning to have a natural childbirth. However, the epidural would make the version more likely to succeed. Rachel asked the nurse if this was his first time performing the procedure. He answered that it was not.
“How many have you performed?” she asked.
“Too many to count,” was the answer. Was she the first person to ask? No, he said with a chuckle, admitting that fortunately the first woman he performed the procedure on did not ask.

The Version
With her belly numb, the external cephalic version could finally begin at 8am. Dr. D and an OB resident began pushing deep into Rachel’s belly in an effort to flip the baby, with a medical student and some nurses looking on. The procedure appeared to require a great deal of athleticism as the doctors dug their hands deep into the belly, so much that the baby was visible to onlookers as a large lump.
The first attempt was unsuccessful. As the second began, I began playing a recording of The Byrds’ song “Turn! Turn! Turn!” for motivation. Although it made Dr. D smile, this attempt, too, was unsuccessful. My feelings of dread, present at low levels this entire morning, grew. This isn’t going to work, I thought to myself.
The third attempt, however, began to see headway. After a great deal of pushing, the vertical lump turned into a horizontal lump. After a quick breather, they continued pushing and the lump became vertical again. Dr. D asked for an ultrasound to confirm that the version had worked. I was still getting my bearings on the ultrasound image when the medical student gave a thumbs up. Belly Buddy was now head down! The entire procedure had taken about 20 minutes.

Induction
The original plan had been to go home if the version was successful. I was surprised when Rachel readily agreed to Dr. D’s suggestion of inducing labor. Neither of us wanted to deal with the prospect of having the baby flip again. Dr. D had to depart for office hours, so the resident placed a Foley bulb to begin dilating Rachel’s cervix.
Around 10:45am, we were transferred to Labor & Delivery Room 11, a spacious room with a varnished wood laminate floor, restroom with shower, an entertainment center sort of like the seat back on an international flight, and a big picture window with a view of…the parking lot. Rachel was transferred to an uncomfortable techno-bed with controls adjusting the bed’s angle and so-called softness.
Around noon, we met CNM (certified nurse midwife) B for the first time. She was to be a reassuring presence during the next two days and the provider who, more than any other, seemed to be on the same page as us. She warned us that the induction could be quite slow and would probably take at least 24 hours.
Although the epidural takes about two hours to wear off, a margin of safety requires patients to wait six before they try to walk, a very long time to stay in bed on IV fluids. What followed was the most amusing anecdote from this entire adventure. Unfortunately, my bride has censored the re-telling of the story. I am authorized only to reveal that the story involved a bedpan, massive quantities of urine, considerable underwater flatulence, and a laughing fit. Not long after this untold tale occurred, she had her first contraction, a low level one that she said felt like a mild menstrual cramp.
A Slow Process
After the six hour limit passed, Rachel was able to have her IV capped off and take some dignity back by changing into a dress that she’d bought with labor in mind. Later in the afternoon, Dr. D came by. She concurred with CNM B that nothing was going to happen tonight. The Foley fell out around 5pm, indicating Rachel was 3 cm dilated.
I joined my parents and Rachel’s mother for dinner at Don Pablo’s. The restaurant wasn’t too far away from the hospital and was usually quick. Ironically the kitchen’s speed was abysmal this particular day. Our server sheepishly admitted that the kitchen manager had recently defected to a rival Mexican restaurant, taking half the kitchen staff with him.
We brought a steak taco salad and cup of chicken tortilla soup back for Rachel. The overnight OB, Dr. G stopped by while she was eating. Although Dr. D’s orders authorized Rachel to eat in the evening, Dr. G seemed cranky about either her choice of meal or the fact that she was eating in the first place. Rachel and the doctor discussed the scientific merit of people fasting before they need to do some prolonged athletic activity (including giving birth).
He countered my wife’s argument—that being well nourished was worth the risk of stomach upset—with something along the lines of, “You know, there’s a reason they say you shouldn’t eat for an hour before swimming.” The statement referenced the old canard that a child who goes swimming immediately after eating would get cramps and drown. We couldn’t believe a doctor apparently still believed there was some truth to that!
(The seemingly random swimming reference began to make more sense the following day. When we told the story to CNM B, she laughed and mentioned that Dr. G was about to fly down to Rio where he would be serving as an official for swimming events in the Olympics!)
Kelly Clarkson’s “Heartbeat Song” (especially the lyrics “up up up up all night long, oh up up all night long”) took on new meaning when we were trying to sleep that evening. The nurses forgot to turn the baby’s monitor volume down. In addition to the loud heartbeats, the baby kept kicking the monitor, making a loud, intermittent thump that made it difficult to sleep until the nurse came back to turn it down.
TUESDAY
With the Foley out, Rachel was supposed to start on a regimen of Pitocin, a synthetic oxytocin that would hopefully induce her uterus to have more contractions. Starting at 2:30am, the dosage was supposed to be increased every half hour, but it seems the overnight nurses got busy or forgot because the dosage was only increased once during the entire night.
Dr. D stopped by again in the morning. Unfortunately, Rachel’s cervix hadn’t dilated any more on its own beyond what the Foley had done the day before. It was a slow, frustrating day during which contractions induced by the Pitocin continued frequently but at very low levels. My parents hadn’t packed for the long haul and had to head home. The one silver lining was our friendly evening nurse, who went by the nickname “Mashed Potatoes” because of her unwieldy Zimbabwean surname. She was in our room quite a lot, either because we were her favorite patients or because baby’s “extreme fetal movement” necessitated constant re-positioning of the baby monitor.
The Pitocin was discontinued at 8pm for a few hours, a technique referred to as “Pit Rest”. Rachel was able to get up for a few hours and leave the room for the first time since arriving on Monday. Since we couldn’t leave the two hallways that made up the labor and delivery area, Rachel quickly grew bored of just walking. Extending her hand, we entered a dance frame and waltzed down the hallway. (We also tried one salsa turn pattern before deciding that it was a bad idea due to the flailing capped off IV lines.)
Some of the nurses asked where we danced. We explained that we took lessons at Take the Lead up in Hockessin and had lately been dancing at Delaware Park Casino. The casino, practically across the street from the hospital, has free Latin dancing on Sunday nights. A few Sundays ago, an older woman on the sidelines asked Rachel when she was due. Rachel told her.
“And you’re bouncing around like that? That baby’s gonna fall out on the floor!” the woman said with outraged indignation. Recounting this story to the amused nurses, I commented that it sounded like a far less tedious labor than what we were experiencing now.

WEDNESDAY
We got the most sleep we’d gotten since Saturday night, interrupted only when a nurse started the Pitocin back up at 2am. Come morning, we learned from a new OB and CNM that Rachel was barely more dilated than she had been on Monday evening. They gave us two options. They could try to break the bag of waters and hope it stimulated a progression of labor, though there seemed to be little scientific evidence that would happen and it would start the clock ticking towards ending up with a c-section. The second option was that we could go for a biophysical ultrasound and if everything checked out with the baby, be discharged to see if Rachel would just go into labor on her own time. The latter had been our original plan on Monday. The fact that baby had stayed head down this long made us hopeful that the baby wouldn’t flip again once we headed home.
Belly Buddy passed the biophysical ultrasound with flying colors; even the amniotic fluid level was the best level it had been in months. Afterward, it was just a matter of removing her IV and epidural hardware and signing the discharge paperwork. Rachel remarked that nothing during this adventure had gone according to her birth plan, right down to going home with a fetus instead of a newborn. Although we may have made the same decisions, I do think we should have been told in advance that inductions fail about half the time in women over 30.

In the grand scheme of things, the ordeal was a small one compared with what it must be like to have a high risk pregnancy or unhealthy newborn. Looking back, the silver lining of our experience was memories of the amusing if farcical moments and the inspirational, dedicated medical providers we met. That bittersweet mixture of joy and frustration is one that I suspect will become quite a familiar one on the road of parenthood.
